MEDICAL INFORMATION AND SELF HELP
- SLEEP APNEA! DO YOU NEED TREATMENT?
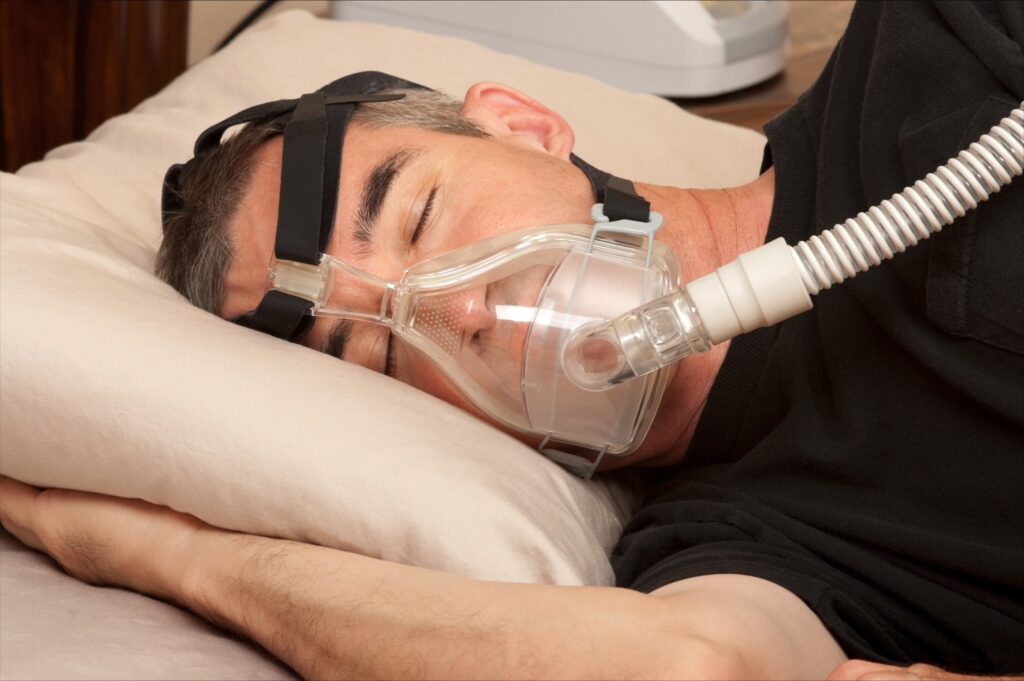
- Already Use CPAP?
- EDUCATION VIDEOS
- PATIENT FORMS
What is Sleep Apnea?
What Causes Sleep Apnea?
Sleep apnea can have various causes depending on the type and severity of the condition. Some common factors that can contribute to sleep apnea are:
• Obesity: Excess weight can put pressure on the throat muscles and cause them to collapse during sleep, leading to OSA.
• Anatomy: Some people have narrow airways, enlarged tonsils, or a deviated septum that can obstruct the airflow during sleep.
• Age: As people get older, their muscle tone and tissue elasticity decrease, making them more prone to OSA.
• Gender: Men are more likely to have sleep apnea than women, especially before menopause.
• Family history: Sleep apnea can run in families, suggesting a genetic predisposition to the disorder.
• Smoking: Smoking can increase inflammation and fluid retention in the throat, which can worsen OSA.
• Alcohol and sedatives: These substances can relax the throat muscles and interfere with the brain’s signals to breathe, causing CSA or worsening OSA.
• Medical conditions: Some medical conditions, such as heart failure, stroke, brain injury, or neuromuscular disorders, can affect the brain’s ability to regulate breathing and cause CSA.
What are the Symptoms of Sleep Apnea?
Sleep apnea can have many symptoms that can affect a person’s quality of life and well-being. Some common symptoms of sleep apnea are:
• Loud and chronic snoring: Snoring is a sign of airway obstruction and can indicate OSA. However, not everyone who snores has sleep apnea, and not everyone who has sleep apnea snores.
• Gasping or choking during sleep: These are signs of breathing interruptions that can occur in both OSA and CSA.
• Daytime fatigue and sleepiness: People with sleep apnea often feel tired and sleepy during the day because they do not get enough restful sleep at night. This can affect their mood, concentration, memory, and performance at work or school.
• Morning headache: People with sleep apnea may wake up with a headache due to low oxygen levels in the blood and high carbon dioxide levels in the brain.
• Dry mouth or sore throat: People with sleep apnea may breathe through their mouth during sleep, which can cause dryness or irritation in the mouth or throat.
• Mood changes: People with sleep apnea may experience depression, anxiety, irritability, or mood swings due to poor sleep quality and chronic fatigue.
• High blood pressure: Sleep apnea can cause blood pressure to rise due to stress on the heart and blood vessels from low oxygen levels and frequent arousals during sleep.
• Heart problems: Sleep apnea can increase the risk of heart attack, stroke, arrhythmia, or heart failure due to its effects on blood pressure, oxygen levels, and inflammation.
An Alternative if CPAP Isn’t Your Thing.
While CPAP therapy is recognized as the gold standard for controlling obstructive sleep apnea, it’s not always feasible or desired by every patient. This is where custom-fitted oral appliances come in as a viable alternative treatment approach for mild-moderate cases.
Dentists skilled in dental sleep medicine use impressions of your teeth to craft a precise-fitting device, much like a customized sports mouthguard. Worn during sleep, it holds the lower jaw slightly forward to keep the airway propped open. This prevents the tongue and soft tissues from obstructing normal breathing patterns.
Early research has found these removable appliances effectively reduce apnea events and daytime sleepiness comparable to CPAP therapy in motivated patients. More recent studies continue supporting oral appliances as an option able to significantly enhance the quality of life for those who either cannot acclimate to or simply prefer avoiding the nightly use of pressurized airflow.
While CPAP remains the first-line defense in clinical guidelines, personalized oral appliances manufactured by an experienced dentist offer a viable alternative for managing mild sleep apnea or serving as a backup plan. A thorough consultation can determine if this more comfortable option may work well alongside lifestyle modifications and management of underlying risk factors in your individual case. Compliance and follow-up remain key to long-term success with either approach.


